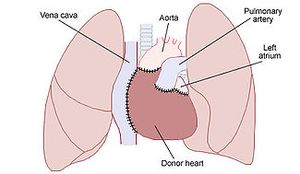
زراعة القلب
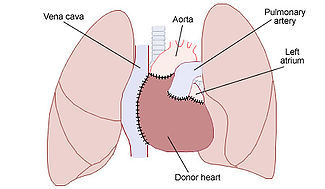
Heart transplantation, or cardiac transplantation,عمليات زرع القلب عمل جراحى transplant تجرى للمرضى في المرحلة الأخيرة من heart failure خطير مرض شرياني تاجي. أغلب العمليات الشائعة هو بنقل قلب صحيح يعمل heart من شخص يكابد الموت أو مشرف على الموت organ donor (allograft)و زرعه في صدر مريض. إما أن يكون قد أزيل قلبه من الصدر (orthotopic procedure) أو , بصورة غير شائعة, يترك لدعم القلب المزروع (heterotopic procedure); كلاهما حلولا مقبولة لواحدة من أكثر المشاكل الصحية حرجا . الفترات المتاحة للحياة أعقاب تلك العمليات تصل الى 15 عاما.<refailments name="2007 documentary">Till Lehmann (director). The Heart-Makers: The Future of Transplant Medicine (documentary film). Germany: LOOKS film and television. {{cite AV media}}: Unknown parameter |year2= ignored (help)</ref>
وحول العالم تبلع العمليات التى تجرى سنوياحوالى 3,500 عملية زرع قلب ,أو نقل قلب ; ويوجد حوالى 800,000 شخص لديهم عيب في القلب من الفئة الرابعة IV (moribund) ويحتاجون الى زرع قلب.[1] This disparity has spurred considerable research into the use of non-human hearts since 1993. It is now possible to take a heart from another species (xenograft), or implant a man-made artificial one, although the outcome of these two procedures has been less successful in comparison to the far more commonly performed allografts. Engineers want to fix the remaining problems with the manufactured options in the next 15 years.[2]
التاريخ
قام فريق من الجراحين بجنوب إفريقيا بقيادة الجراح كريستيان برنارد بعملية زرع قلب إنسان في العام 1967م، وعاش المريض لمدة 18 يومًا ومات بعدها بسبب التهاب رئوي.
وفي أواخر الستينيات وأوائل السبعينيات من القرن العشرين الميلادي أجرى الأطباء عدة عمليات لزرع قلوب. ولكن معظم المرضى ماتوا في السنة الأولى لأن الجسم كان يرفض العضو الغريب، حتى كاد الأطباء أن يوقفوا عمليات زرع القلب. وفي الثمانينيات من القرن العشرين بدأ الأطباء باستعمال دواء يسمى سيكلوسبورين ليقاوم رفض الجسم للعضو الغريب. وكان هذا الدواء سببًا ـ بمشيئة الله ـ في إطالة الحياة بعد العملية عند المرضى. وصارت المشكلة الرئيسية في عمليات زرع القلب هي قلة وجود متبرعين.
حدث تقدم سريع في العلاج والوقاية مع التقدم الهائل في عمليات زراعة القلب، وطور الأطباء مُحْصِرات البيتا في أواخر الستينيات من القرن العشرين، وهذه الأدوية تساعد على خفض ضغط الدم المرتفع وتمنع الذبحة وتتحكم في بعض أنواع اللانظمية. أما مُحْصِرات قنوات الكالسيوم التي تعمل مثل مُحْصِرات بيتا فقد ظهرت في السبعينيات من القرن العشرين.
أجرى الطبيب السويسري أندرياس جروينتزج أول عملية ترقيع وتقويم للأوعية في العام 1977م، وهي عملية غير جراحية في طبيعتها وتُجرَى لفتح أي شريان مسدود. وطور الباحثون تقنيات أخرى تستعمل مع تقويم وترقيع الأوعية لتزيد من فاعليتها. وصار مزيل الرجفان المزروع متوافرًا منذ سنة 1985م. وهو جهاز يحدد الانقباضات الزائدة في البطين ويرسل شحنة كهربائية صغيرة لوقفها.
وتركزت مقاومة ومنع أمراض القلب في تقليل عوامل الخطر التي يمكن التحكم بها. ومن الأسباب الرئيسية للإصابة بمرض الشرايين التاجية فرط ضغط الدم المرتفع وارتفاع نسبة الكولسترول في الدم وتدخين السجائر، والتحكم في هذه العوامل قد يمنع تطور المرض.
إن معظم الذي تعلمناه لمنع أمراض القلب مصدره الأبحاث الطبية المكثفة. فقد أعطتنا دراسة فرامنجهام مثلاً، للقلب معلومات وافية عن عوامل الخطر التي تخص أمراض الشرايين التاجية. وبدأت الدراسة في عام 1948م في فرامنجهام بولاية ماساشوسيتس الأمريكية، وفحصت قلوب خمسة آلاف شخص. وبفضل هذه البحوث وغيرها طور العلماء أدوية جديدة لعلاج ضغط الدم المرتفع وارتفاع نسبة الكولسترول في الدم.
وعمل كثير من الناس على تحسين حالة قلوبهم بتعلم أساليب الطب الوقائي، كأن يقوموا بقياس ضغط الدم وقياس نسبة الكولسترول بانتظام. ومعظم الذين يشكون من ارتفاع طفيف في ضغط الدم حافظوا على أخذ كمية قليلة من الملح وكميات قليلة من السعرات الحرارية في الوجبات الغذائية. وبعضهم قلل نسبة الدهون المركزة في وجبتهم، وزيادة على ذلك فإن هناك أعدادًا متزايدة تمارس التمارين الرياضية، وذلك يساعد على تخفيف الوزن وبالتالي يقلل نسبة الكولسترول ويخفض ضغط الدم.
دواعى الجراحة
In order for a patient to be recommended for a heart transplant they will generally have advanced, irreversible heart failure with a severely limited life expectancy. Other possible treatments for their condition, including medication, should have been considered prior to recommendation. Generally, the following causes of heart failure can be treated with a heart transplant:
- Cardiomyopathy
- Congenital heart disease
- Coronary artery disease
- Heart valve disease
- Life-threatening arrhythmias.
Contraindications
Some patients are less suitable for a heart transplant, especially if they suffer from other circulatory conditions unrelated to the heart. The following conditions in a patient would increase the chances of complications occurring during the operation:
- Kidney, lung, or liver disease
- Insulin-dependent diabetes with other organ dysfunction
- Life-threatening diseases unrelated to heart failure
- Vascular disease of the neck and leg arteries.
- High pulmonary vascular resistance
- Recent thromboembolism
- Age over 60 years (some variation between centres)
- Alcohol or drug abuse
الجراحات
ما قبل العملية
A typical heart transplantation begins with a suitable donor heart being located from a recently deceased or brain dead donor. The transplant patient is contacted by a nurse coordinator and instructed to attend the hospital in order to be evaluated for the operation and given pre-surgical medication. At the same time, the heart is removed from the donor and inspected by a team of surgeons to see if it is in a suitable condition to be transplanted. Occasionally it will be deemed unsuitable. This can often be a very distressing experience for an already emotionally unstable patient, and they will usually require emotional support before being sent home. The patient must also undergo many emotional, psychological, and physical tests to make sure that they are in good mental health and will make good use of their new heart. The patient is also given immunosuppressant medication so that their immune system will not reject the new heart.
العملية
Once the donor heart has passed its inspection, the patient is taken into the operating room and given a تخدير عام. Either an orthotopic or a heterotopic procedure is followed, depending on the condition of the patient and the donor heart.
Orthotopic procedure
The orthotopic procedure begins with the surgeons performing a median sternotomy to expose the mediastinum. The pericardium is opened, the الأوعية الكبرى are dissected and the patient is attached to cardiopulmonary bypass. The failing heart is removed by transecting the great vessels and a portion of the left atrium. The الأوردة الرئوية are not transected; rather a circular portion of the left atrium containing the pulmonary veins is left in place. The donor heart is trimmed to fit onto the patients remaining left atrium and the great vessels are sutured in place. The new heart is restarted, the patient is weaned from cardiopulmonary bypass and the chest cavity is closed.
Heterotopic procedure
In the heterotopic procedure, the patient's own heart is not removed before implanting the donor heart. The new heart is positioned so that the chambers and blood vessels of both hearts can be connected to form what is effectively a 'double heart'. The procedure can give the patients original heart a chance to recover, and if the donor's heart happens to fail (eg. through rejection), it may be removed, allowing the patients original heart to start working again. Heterotopic procedures are only used in cases where the donor heart is not strong enough to function by itself (due to either the patients body being considerably larger than the donor's, the donor having a weak heart, or the patient suffering from ارتفاع ضغط تنفسي).
ما بعد العملية
The patient is taken into ICU to recover. When they wake up, they will be transferred to a special recovery unit in order to be rehabilitated. How long they remain in hospital post-transplant depends on the patient's general health, how well the new heart is working, and their ability to look after their new heart. Doctors typically like the new recipients to leave hospitals soon after surgery because of the risk of infection in a hospital (typically 1 - 2 weeks without any complications). Once the patient is released, they will have to return to the hospital for regular check-ups and rehabilitation sessions. They may also require emotional support. The number of visits to the hospital will decrease over time, as the patient adjusts to their transplant. The patient will have to remain on lifetime immunosuppressant medication to avoid the possibility of rejection. Since the vagus nerve is severed during the operation, the new heart will beat at around 100 bpm until nerve regrowth occurs.
زراعة 'عضو حي'
Doctors made medical history in February 2006, at Bad Oeynhausen Clinic for Thorax- and Cardiovascular Surgery, ألمانيا, when they successfully transplanted a 'beating heart' into a patient.[3] Normally a donor's heart is injected with potassium chloride in order to stop it beating, before being removed from the donor's body and packed in ice in order to preserve it. The ice can usually keep the heart fresh for a maximum of four[4] to six hours with proper preservation, depending on its starting condition. Rather than cooling the heart, this new procedure involves keeping it at body temperature and hooking it up to a special machine called an Organ Care System that allows it to continue beating with warm, oxygenated blood flowing through it. This can maintain the heart in a suitable condition for much longer than the traditional method.
الأعراض
The prognosis for heart transplant patients following the orthotopic procedure has greatly increased over the past 20 years, and as of May 30, 2008, the survival rates were as follows.[5]
- 1 year: 87.5% (males), 85.5% (females)
- 3 years: 78.8% (males), 76.0% (females)
- 5 years: 72.3% (males), 67.4% (females)
In a November 2008 study conducted on behalf of the U.S. federal government by Dr. Eric Weiss of the Johns Hopkins University School of Medicine, it was discovered that heart transplants- all other factors being accounted for- work better in same-sex transplants (male to male, female to female). However, due to the present acute shortage in donor hearts, this may not always be feasible.
As of the end of 2007, Tony Huesman is the world's longest living heart transplant patient, having survived for 29 years with a transplanted heart. Huesman received a heart in 1978 at the age of 20 after viral pneumonia severely weakened his heart. The operation was performed at Stanford University under American heart transplant pioneer Dr. Norman Shumway, who continued to perform the operation in the U.S. after others abandoned it due to poor results.[6]. Another noted heart transplant recipient, Kelly Perkins, climbs mountains around the world to promote positive awareness of organ donation. Perkins is the first heart transplant recipient to climb to the peaks of Mt. Fuji, Mt. Kilimanjaro, the Matterhorn, Mt. Whitney, and Cajon de Arenales in Argentina in 2007, 12 years after her transplant surgery. Dwight Kroening is yet another noted recipient promoting positive awareness for organ donation. Twenty two years after his heart transplant, he is the first to finish an Ironman competition.[7] Fiona Coote was the second Australian to receive a heart transplant in 1984 (at age 14) and the youngest Australian. At 24 years since her transplant she is also a long term survivor and is involved in publicity and charity work for the red cross, and promoting organ donation in Australia.
The record for heart transplant longevity in a senior recipient may go to Edward Daunheimer of Newburyport, Massachusetts, who received his heart on 19 February 1997 at the Tufts New England Medical Center at the age of 65 (the upper age limit for heart transplants).[بحاجة لمصدر] Mr. Daunheimer has so far lived a healthy life for 12 years with his new heart, defying statistical probabilities by a large margin.[بحاجة لمصدر]
المصادر
- ^ Reiner Körfer (interviewee). The Heart-Makers: The Future of Transplant Medicine (documentary film). Germany: LOOKS film and television.
{{cite AV media}}: Unknown parameter|year2=ignored (help) - ^ خطأ استشهاد: وسم
<ref>غير صحيح؛ لا نص تم توفيره للمراجع المسماة2007 documentary - ^ "Bad Oeynhausen Clinic for Thorax- and Cardiovascular Surgery Announces First Successful Beating Human Heart Transplant". TransMedics. 23 February 2006. Retrieved 2007-05-14.
- ^ Custodiol Htk Solution patient advice including side effects
- ^ Heart Transplants: Statistics The American Heart Association. Retrieved 28 February 2009.
- ^ Heart Transplant Patient OK After 28 Yrs (14 September 2006) CBS News. Retrieved 29 December 2006.
- ^ Dwight Kroening first heart transplant to do ironman Retrieved 27 August 2008.
- Western Cape government, South Africa (21 February 2005). "Chris Barnard Performs World's First Heart Transplant". Cape Gateway. Retrieved 2007-01-10.
- Department of Cardiothoracic Surgery. "Patient's Guide to Heart Transplant Surgery". University of Southern California. Retrieved 2007-01-10.
- Nancy Reid (22 September 2005). "Heart transplant: How is it performed?". Healthwise. Retrieved 2007-01-10.
- Jeffrey Everett (2003-10-29). "Heart Transplant: Indications". AllRefer.com. Retrieved 2007-01-10.
- "Hartford Hospital Heart Transplant Program". Hartford Hospital, Connecticut, United States. Retrieved 2007-01-10.